Two weeks ago my investigative feature about surgeons violating breast cancer patients’ requests to go flat went up on Cosmopolitan.com. In the days following, my social media channels were inundated with #MeToo testimonies from breast cancer survivors as well as messages from readers and supporters who had no idea that women’s bodies were being abused and disrespected in this way. I have been buoyed by supportive messages, tweets, and posts. Thank you!!!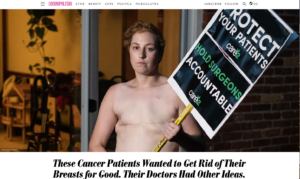
The highlight was an email I received yesterday from Dr. Patricia Clark, a nationally recognized breast surgeon in Arizona who was quoted in the piece. (For context: Dr. Clark travels the country teaching surgeons how to make women truly flat after mastectomy. She is my new hero.)
Dr. Clark gave me permission to share the email she wrote me:
Hi Catherine,
I thought you’d like to know…I was speaking at an international advanced oncoplastic surgery course over the weekend and your article was put up on the screen by the surgeon doing the opening introductory speech emphasizing respect for patient choice. It was presented and referenced several times during the conference with the photo of the patient [Kim] holding the sign demanding surgeon accountability…
My heart skipped a beat when I read her note. I was in my (parked) car. Rain pounded on the roof. A chill crept through my body as water soaked through my jeans, wet from dashing to my car through a downpour (the last gasp of Hurricane Florence as it moved through Massachusetts).
In my 20+ years as a women’s health journalist, I’d never felt more gratified than I did in that chilled, rain-soaked moment. I thought of Kim Bowles, the brave, badass woman who refused to go quietly. Of the hours she and I spent on the phone, trying to get the story right. Of the power of the media to shine a light of truth on women’s stories.
To amplify women’s voices so they were heard by a room full of international surgeons capable of affecting change on a global scale. To imagine even a single doctor who may feel compelled to listen closely, to attune to a woman’s voice, hear her autonomy, and respect her choice, made all I’ve been through as both a patient and a women’s magazine journalist worth it.
Thank you to those who trusted me with your stories: Kim Bowles, Becky Fitz, BethAnne King and so many more who shared their painful truths with me but, due to space limitations, weren’t named in the story. You are also my heroes.
Yesterday, Kim Bowles and I sat down for a joint interview about the Cosmo story and about my new memoir, FLAT. We spoke to the smart and engaging Megan Harris, the producer/director for The Confluence, 90.5 WESA, an NPR station in Pittsburgh, PA. (The interview was recorded, and I will post a link when it goes live.)
In the meantime, stay tuned for more news from me and Kim as we have some exciting things in the works!

